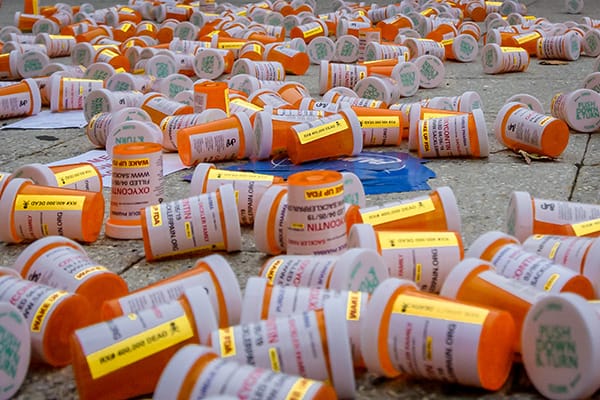
Credit: Nick YoungsonCC BY-SA 3.0Pix4free
I once worked for a black-owned and operated psychiatry practice and pain management clinic in Las Vegas that served exclusively Medicaid patients. As I quickly learned, Medicaid is rife with fraudulent billing. It’s a jackpot for people who are willing falsely to claim they served patients or who provided services patients didn’t want or need.
I was put on the newly established case management team along with two other new hires: a cocky, fat black man and a sweet black woman who had been a college track star. Our boss was a fat, second-generation Haitian woman.
Our job was to figure out what kinds of help our clients needed and put them in touch with community-based services for which Medicaid was willing to pay. The idea was to be an advocate for clients who were presumably too disabled to do this on their own. We started with training exercises, and I quickly learned that my job was to bill for imaginary services or greatly pad any actual services provided.
For example, we were to pick a patient who had an upcoming appointment for psychiatry or pain management and telephone to confirm the appointment. We actually did make the call, but often there was no answer or we just left a message. We would then write fraudulent case-management notes that might read something like this: “Case manager provided scheduling assistance for the patient’s next pain management and therapy appointment and linked patient to community services for food assistance.”
We then billed for two hours of work, whether we spoke to the patient or not. Medicaid would get the bill — and pay it. The agency was probably billing Medicaid $65 an hour for case management. We got $25 an hour, and the agency pocketed the rest, so the agency wanted as much of this “work” out of us as possible.
It may seem incredible that the agency can get away with this kind of fraud, and Medicaid does try to control it. However, once an agency is qualified as a Medicaid-certified service provider, the assumption is that all charges are justified. There is such a huge volume of payments going through the system that unless there is something egregiously, obviously wrong with them, no one is likely to check.
We soon learned that the agency had not set aside a training budget for us, as any normal company would have. Our pay came exclusively from fraudulent billings.
The fat black man on our team didn’t seem to think there was anything wrong with this, but the sweet black woman and I were very uncomfortable about it. She was afraid to complain to our boss, the Haitian woman, who had a chip on her shoulder and an irritable demeanor. So, I talked to the boss. She angrily told me to go back to my office and do my job. I had no business asking questions like that.
Our little team of three was in a small office in the back corner of the smaller of two buildings that made up the practice. Our boss told us never to leave our office and never to go into the other, larger building, where the doctors and nurses worked. It was she who had started the “case management” group, and in retrospect, she seemed to be trying to hide us from the rest of the practice. Our team was set up as a fraud from the start, and she may have been afraid that others in the practice might find out what a scam it was and complain.
Later, I found out that the black doctor who owned the practice had at first objected to getting into case management because he knew our job was to pad bills. If there was enough fraud to make Medicaid suspicious, it could investigate us, and theoretically shut down the practice. My guess is that the Haitian talked him into it because of the prospect of so much easy money. In any case, we were under orders never to talk to anyone about what we did. “Case management” appeared to be a dirty little secret.
Patients the agency was treating for pain management always showed up for appointments. They loved getting the drugs, and the clinic was building a reputation for overprescribing addictive pain medicine. The problem was trying to get all the patients through the door. Most days, the waiting room was jammed with people sometimes with a line stretching out the door.
Credit Image: © Erik McGregor/ZUMA Wire
The visits with doctors and nurses for pain management lasted no more than 15 minutes. This is unethical medical practice, because there is no way adequately to assess pain, review history, do drug tests if necessary, explain risks, and exchange information. Patients were in and out the door so the practice could bill for as many treatments as possible. If patients became addicted, well, that just meant they became loyal clients. Addicts build up a tolerance to drugs, which means they need more pills. Every prescription the agency wrote meant more revenue. I didn’t work in billing, so I don’t know what the cut was, but it was enough to be a strong incentive to write as many prescriptions as possible.
Were some of our patients selling their drugs on the black market? Definitely. The agency had to worry about this because if painkillers were traced back to them, there could be trouble. One measure against this was to do a test on patients to see if they had the drug in their systems. If they were negative for pain pills, they were assumed to be flogging the pills, so they wouldn’t get their prescription. The trick to get around that, of course — and I heard of some blacks doing this — was to take a pill the day of the appointment so as to test positive.
When I first went to work there, I didn’t know about any of this.
Las Vegas is only about 12 percent black, but I would say the agency’s total patient mix was about 65 percent black, 30 percent white, and 5 percent other — mostly Hispanics. I never saw an Asian. Black patients tended to be rude, act entitled, and make a stink if things didn’t go their way. For example, if they wanted a certain drug but a prescription couldn’t be written for it, they — both sexes — could get hostile and out of control. A white woman in the same situation would be more likely to cry.
Blacks also broke rules, such as the ban on eating in the waiting room. The staff would make others stop eating, but would not enforce rules against blacks for fear of a blow-up.
Unlike patients for pain management, who loved to come in for their drugs, patients for therapy, needs assessments, or physicals were a different story. We couldn’t get them to come, and every appointment was agency revenue. Most wouldn’t bother to cancel, so the practice had to waste time holding appointments open that could have gone to someone else. We even went so far as to pay for Lyft rides, but many patients refused to get out of bed or leave their homes. The drivers would show up, wait a while, call the practice, and tell us they were leaving. We would have to pay the drivers anyway. We had a transportation team that would show up in nice vans with snacks on board. That wouldn’t get patients out their doors, either.
When blacks did come to their doors for a ride, they were like the blacks in the waiting room: rude, complaining, prone to outbursts. If the driver was late, they would complain to our agency to the point of getting the driver fired.
In any case, our “case management” group was told to solve the problem of getting these people to their appointments. We had divided up the city of Las Vegas into five zones, with different drivers working in different zones, trying to bring in patients. One day, during a meeting of our group, I had a disagreement with the cocky black man. There was a poor part of town to which I wanted to allocate more drivers, but most of the drivers were white. He wanted to assign driving duties to black case managers, even though it wasn’t their job to drive patients around. As noted, they are supposed to link patients to services.
Downtown Las Vegas. Credit: Ken Lund via Flickr, CC BY-SA 2.0.
I knew very well that if these black case managers started driving patients to appointments, they would bill for work they weren’t supposed to be doing. They would charge per diem, and pad their bills so much, it could lead to an investigation from Medicaid that could get the agency shut down. My black colleague didn’t want to hear any of this. He sat in his corner of the office, seething in anger. When I looked away, he threw a dry-board eraser across the room and hit me in the back of the head. Then he stood up and threw his chair across the room and challenged me to a fight. This so terrified our black colleague, she had a panic attack. I complained about this incident to our supervisor; she did nothing.
I had to get out of this corrupt case-management group. I thought maybe it was just a bad part of a practice that was otherwise well run. I started talking to the nursing-home team, which was half white and half black. I had a clinical background, and would be a perfect fit. My job would be to visit patients and assess them for dementia (which we euphemistically called neurocognitive disorder). I would then send my assessment notes to the clinical staff at our agency so they could decide on the best treatment. The people in the department said it was challenging and rewarding work, but first I had to get out of case management.
When my Haitian supervisor found out I wanted to leave, she burst into our office and began screaming at me in front of my coworkers. “You think you can leave my team on your own terms behind my back like this!?” “Who the hell do you think you are!?” She grabbed the company-provided Dell laptop out of my hands and took it away. She said it was for case managers, not traitors.
I managed to get out of case management, and into the nursing-home group, where I learned how to do tests for dementia. I would ask them what year it was, where we were, why they were in the home, who was president? Someone with advanced dementia might very well say “JFK.” If the patient was coherent, I got other information, such as family background, criminal record, health, employment history, etc.
Each assessment took about an hour and it took another hour to upload my notes. That meant I could do three or four assessments each day. An important part of my job was to find out if the patient was on psych meds, and to make sure to recommend them if he had “neurocognitive disorder.” That was so my agency could write more prescriptions and make more money.
On my first visit, I checked in at a nursing station and got strange looks, as if I had no right to be there. I called my supervisor, who said I should never talk to nurses; just find a list of newly admitted Medicaid patients, go to their rooms and evaluate them. I found this very strange, but did what I was told.
One day, while I was assessing a paraplegic black man with dementia, a family member walked in. She was angry. She wanted to know who had authorized me to evaluate this severely disabled person without proper consent. That was a fair question. I explained who sent me, why I was there, and gave her my card. The next day, the practice put the nursing-home team on a two-week leave of absence without pay until “things were straightened out.” This may be hard to believe, but the practice I was working for was doing these assessments without authorization from the patient or the facility and was charging Medicaid.
A few weeks later, we were called back in to discuss a new protocol, but it did not appear that any of the kinks in permissibility had been straightened out. The black doctor who ran this part of the business told us only which patients we should avoid and which rehab centers were off limits; nothing about the ethics or legality of what we were doing. He assured us repeatedly that everything was fine.
I never found out what happened during those two weeks. Did the agency work out a deal with certain nursing homes and rehab centers to keep letting us in for those unwanted, unasked-for services? Did they get kickbacks? I didn’t stay long in that department because here, too, it all smelled of fraud. But I remember one unusual patient.
He was a black man I was supposed to assess, but he refused to put his clothes on and was screaming and writhing in bed. He was grunting and screaming, so it was impossible to get any information from him. My boss told me to write up an assessment anyway, and just report what I had seen. There were the usual sections — drug-taking, psychiatric illness, education, family history — which I obviously couldn’t fill in because I hadn’t learned anything. My boss told me just to write “not known,” and turn in what was essentially a useless report. The practice got paid for it.
A different job I had at the practice was called psychosocial rehabilitation (PSR). This is supposed to teach a patient such things as relationship building, interpersonal communication, positive affirmations, community service, and how to get a job. This is supposed to be a supplement to therapy and drugs and is limited to no more than 24 to 36 months, with the idea that the patient will become able to support himself.
This almost never works. Many of these people have been on some form of social support all their lives. The idea of having a job and a boss terrifies them. Even if they were capable of holding a paying job — and most were not — there were enough social programs to live on. So why work? In my career, I had only one notable success: a white woman whose case I described elsewhere.
Therefore, although what I was doing was largely a waste of time, I couldn’t detect any outright fraud. We were following Medicaid rules, providing services, and making money for the agency. But I did meet some interesting people.
My first PSR patient was a black woman diagnosed with bipolar disorder and cocaine addiction. The diagnostic categories don’t make a distinction between powder cocaine and crack-smoking, though the latter is more serious and associated with crazy behavior. She was a crack smoker. She also hung around gas stations and drank something called Four Loko, which was eventually reformulated because it contained both caffeine and alcohol, which raises ethical and legal questions. It made her aggressive.
Credit Image: © Mariela Lombard/ZUMApress.com
She was living in rent-controlled low-income housing and paying rent with the Social Security Disability Income checks she got for being crazy. She was being evicted for throwing a garbage can at her neighbor, and for spreading garbage in and around her home. My boss told me to find a new place for her. When I visited her, the apartment was a filthy mess, with cigarette butts piled up on the floor and cockroaches in the kitchen. She had a litter box full of cat droppings, but no cat.
It was hard to understand this patient because she had only one tooth, had a lisp, and was often drunk. She promised that if she got a new place, she would behave. As her PSR worker, it was my job to persuade the staff of the new place to let her in, and to explain the facility rules in a way she could understand. I got her in.
On follow-up visits, I heard she was foul-mouthed and screamed racial slurs at the top of her lungs — “These white mutha****as on my last nerve!” — which terrified the other residents. I was supposed to change her behavior by teaching her “empathy skills building” — how to be helpful and mindful of other people’s feelings — but that, of course, went nowhere. Within two months, she attacked her white roommate in her sleep. She grabbed a candelabra and repeatedly bashed the poor woman’s skull, fracturing it. I didn’t follow her case after that, but she was kicked out of the facility and I assume she went to jail.
I got a new PSR patient, a homeless black man with a diagnosis of serious schizoaffective disorder. He believed he was getting orders from the government through radio frequencies and television programs. He was getting a total of $1,700 a month — a lot for a bum — from the Veterans Administration and Social Security. He liked being homeless because that would put him beyond the reach of radios and TVs that might order him to do dangerous things.
The practice told me to get him into a halfway house and it handed over $300 in cash of the man’s money to cover the first month’s rent, utilities, and food. Later, I learned that the next day, one of the bum’s friends went to the halfway house pretending to be a case worker. He explained that because of the patient’s delusions and other problems, he would cause trouble and not be safe at the halfway house. The staff gave him the $300. The patient and his pal went on a two-day crack cocaine binge with the money, and we booted the patient out of the practice.
How did the halfway house get tricked into handing over cash to a complete stranger? I don’t know because I wasn’t there, but those places are often staffed with recovering addicts and other dimwits who are not good at checking details.
There were other problems at the agency. Women lodged sexual harassment complaints against the black owner. I never heard of any being proven, but many women complained about him. He was aggressively flirtatious, made comments about women’s clothing, and made jokes with sexual innuendos. After meeting with him, women said they felt violated.
It took me some time to realize it, but the whole agency was rotten with fraud. For the people who ran it, anyone with a blue Medicaid card in his wallet might as well have had a no-limit Amex card. The more unnecessary services the agency could charge the government, the more money it made.
I explained elsewhere how corrupt service providers get friends and family to fake disabilities so they can get on Medicaid. This turns on the money-spigot for government money. It pours in from a bloated federal budget paid for by working citizens. And for any good fraudster, the allure of this deal is that patients don’t get better because they’re not getting quality treatment. The money machine never stops.
You may be asking: Is Medicare really this bad? Is this guy making things up? If he’s not, why aren’t crusading journalists exposing what’s going on? There are several things to consider. First, if insiders spill the beans, they lose their jobs. Only people who have left the business are likely to talk. But even if they name names and state facts, the agency will deny everything, and journalists have no power to compel disclosure.
Something else that will turn up is how much of the fraud is committed by blacks and immigrants. The cases that come to light that are big enough to lead to criminal charges almost always seem to involve non-whites of some kind. Look at the names of the defendants in this case or this or this or this. These people were charging millions of dollars for fraudulent services. Black crooks seem to operate at a lower level, but there are plenty of them, and these are the embarrassing realities that any extensive investigation will uncover.
What we have is not what mental health is supposed to be like. The idea is to help people get back to a normal state of functioning and discharge them in better shape than you found them. But in the wrong hands, it’s a racket. It makes a mockery out of something I believe was set up with good intentions. There must be a private-sector solution to this madness, because government is terrible at catching fraud.
- Post TagsBlacks in Charge, Featured, Race and Health, Welfare